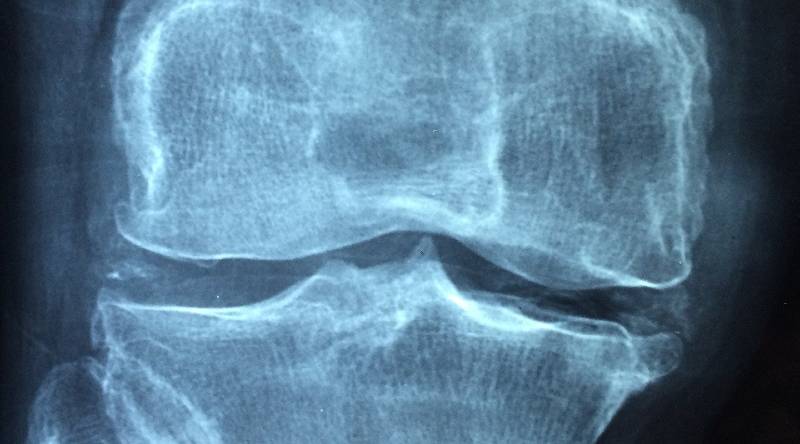
What is Osteoarthritis?
Osteoarthritis of the knee is a painful and degenerative condition where articular cartilage, which acts as a cushion during knee motion, starts breaking down. The aging population is increasing steadily and globally, and it is now predicted to be a major health issue impacting the quality of life and increasing the societal and economic burden for citizens of all ages.
How does pain start in arthritis?
Cartilage covers the ends of the bone in the joints. It distributes body weight and provides a buffer during walking. When normal cartilage is present, bone movement is cushioned. With age or with trauma, the cartilage wears out and becomes irregular, causing the bone ends to grind against each other. When bone touches bone, it is very painful to bear weight as well as to move the joint.
What are regenerative cells?
Regenerative cells are very powerful cells found in the human body. They are what are referred to as precursor cells found mostly in the bone marrow, which can regenerate to any other type of cells (muscle, bone, and cartilage). When regenerative cells are injected into a damaged joint, they can either stimulate or re-form the destroyed cartilage of the knee, fully or partially.1 Furthermore, regenerative cells also decrease inflammation, which decreases pain as well as the progression of the condition.
Are regenerative cells harmful?
No, the regenerative cells are normally present in any human body. The cells are collected from your own body, so the risk of new disease transmission is very negligible. Some patients might develop short episodes of joint swelling, stiffness and mild pain, but this has been found to be non-harmful. Regenerative cell injections are already in clinical use for focal as well as generalized arthritis of the knee, hip, shoulder and ankle. Studies are forthcoming regarding location such as the spine and small joints. It is shown to improve pain, functional status, walking distance and quality of life.
How are regenerative cells administered?
Regenerative cells are taken from the back of the pelvis, after giving proper analgesics. Then, the sample is concentrated by a process called, centrifugation. It is then, either directly injected into the involved joint, or is introduced during various other surgical techniques as a biomechanical scaffold. Sometimes, the regenerative cells are supplemented with additional growth factors from platelet-rich plasma.
Does it work?
There have been studies being conducted throughout the world, regarding the regenerative cells in various diseases, and their use in knee arthritis is also one of them. Most of the studies have found a decrease in pain as well as disease burden1 ultimately improving the sense of well-being for the sufferers. This improvement is often more pronounced in earlier stages of arthritis.1 Regenerative cells can be delivered into a focal lesion where they engraft and assist in joint cartilage repair. Also, these cells can reduce the inflammation within the joint, which is responsible for decreasing the pain and increasing the joint mobility.
To evaluate the outcome after the injection, various pain and function rating scores have been used (e.g., SF-36, VAS, IKDC, etc.), and these scores have been found to have improved significantly, even up to 6 years in some studies.4 Currently, studies are being conducted to learn about the dosing and duration of the benefits after injection. However, it should be noted that the Food & Drug Administration (FDA) considers regenerative cell treatment “investigational”. The devices that spin the bone marrow to concentrate the regenerative cells are FDA-approved centrifuges.
Is it costly?
It depends upon the types and frequency of treatment you require, and generally speaking, it is costlier than other modalities like physiotherapy and steroid injections. However, the costs are minimal compared to the pricing for joint replacement surgery. Regenerative cells are not generally included in insurance policies, and the patient typically has to pay out of pocket. There are, however, some insurance companies that are beginning to consider and even making partial payments for these newer technologies.
Some alternatives to regenerative cell injections:
- Weight loss: more bodyweight means, more load upon the knee and hip. So, weight loss is important for every other treatment to be successful.
- Avoid excessive stair climbing: Using stairs causes more joint pressures, and can increase the rate of wear of the cartilage.
- Over-the-counter analgesics (e.g. acetaminophen): Arthritis of the knee is episodic, so when there is a sharp pain, analgesics will cut-off the pain and can give you longer pain-free interval.
- Steroid injections into the joint: When over-the-counter analgesics do not provide adequate pain relief, then the healthcare provider can provide you with a steroid injection, which acts immediately as well and may provide a pain-free interval.
- Hyaluronic acid into the joint: Hyaluronic acid acts as a joint lubricant, or gel, and is a very similar procedure to a simple steroid injection.
- Physiotherapy: Improving muscle strength around the joint, will improve blood supply, as well as stabilize the joint and this increases healing response within the joint.
- Alternative therapies: yoga, acupuncture, pilates, etc. can be utilized.
The last resort is a partial (Unicompartmental) or full (Total knee replacement), wherein the damaged cartilage is replaced with metal implants, and the alignment is corrected. Knee replacement provides very promising results of decreased pain and increased mobility, but has very lengthy recovery time and requires a review of risks and benefits for a rather extensive procedure.
To Summarize
Regenerative cell injections are a promising treatment for relief of discomfort and cartilage growth. These treatments are already in clinical use for the treatment of arthritic conditions and are best considered to delay more extensive surgery or joint replacement.
References: (in Vancouver format)
1. Qi Y, Feng G, Yan WJMbr. Mesenchymal regenerative cell-based treatment for cartilage defects in osteoarthritis. 2012;39(5):5683-9.
2. Mehrabani D, Jaberi FM, Zakerinia M, Hadianfard MJ, Jalli R, Tanideh N, et al. The healing effect of bone marrow-derived regenerative cells in knee osteoarthritis: a case report. 2016;5(2):168.
3. Kehoe O, Cartwright A, Askari A, El Haj AJ, Middleton JJJotm. Intra-articular injection of mesenchymal regenerative cells leads to reduced inflammation and cartilage damage in murine antigen-induced arthritis. 2014;12(1):157.
4. Orth P, Rey-Rico A, Venkatesan JK, Madry H, Cucchiarini MJSc, advances c, et al. Current perspectives in regenerative cell research for knee cartilage repair. 2014;7:1.
- Get a Grip on Thumb Pain - March 25, 2024
- Spring PRP and Biologics Discount Day - March 18, 2024
- Tennis Elbow, Anyone? How to treat and manage the condition known as Tennis Elbow. - March 13, 2024